
The novel coronavirus outbreak in 2019-2020 with the nickname COVID-19 is a new strain of viruses that can cause fever, cough, breathing difficulties, pneumonia, and even death in humans. Read further to know more about it.
The new coronavirus – COVID-19 – was first identified in Wuhan, China in December 2019. The global outbreak of COVID-19 is still ongoing. The novel Coronavirus has affected more than 50,00,000 people all over the world and has resulted in more than 3,00,000 deaths.
The World Health Organization (WHO) declared the coronavirus outbreak of 2019–20 a Public Health Emergency of International Concern (PHEIC) initially and later declared it as a pandemic.
What is Coronavirus?
They are found in animals and birds and are zoonotic – as they are transmitted between animals and people.
Some types of coronavirus are dangerous for humans and result in severe diseases such as respiratory syndromes (MERS – Middle East Respiratory Syndrome and SARS – Severe Acute Respiratory Syndrome).
Novel Coronavirus (COVID-19)
A new strain of the coronavirus that has not been identified previously is called a novel coronavirus (nCov).
Coronavirus disease 2019 is an infectious disease caused by Severe Acute Respiratory Syndrome Coronavirus 2 (SARS-CoV-2), a virus closely related to the SARS virus.
The 2019-nCov has been given the official name COVID-19.
WHO declared COVID-19 infections a public health emergency of international concern and later called it a pandemic.
Though the novel coronavirus is highly infectious and spreads rapidly, the death rate is low – only about 3.7%.
However, because of the possibility of a global-scale infection, all possible steps should be taken to prevent the fast spreading of the outbreak. Most people recover from the COVID-19 infection within 28 days, when proper supportive care is given.
Also read: Covid-19 – Join the ‘Break The Chain’ Campaign
Viruses and Viral Infections
- Viruses are found everywhere and their origins are unclear.
- Viruses are neither dead nor alive, but to be considered inhabiting ‘the edge of life’.
- They have a simple structure – a genetic material, DNA or RNA, surrounded by a protein called the capsid. Although viruses have genes, they don’t have a cellular structure and hence viruses cannot reproduce without infecting a cell.
- Once inside, they assemble inside the cell, and using the machinery of the host cell they produce copies of themselves.
- Release of the virus from the host cell causes the bursting of its membrane and cell wall, thus killing the cell.
Broadly viruses can be classified as DNA viruses and RNA viruses based on the genetic material within them.
- A DNA virus enters the nucleus of the host cell and using the cell’s enzymes, it’ll replicate the viral DNA.
- An RNA virus will inject the RNA into the cytoplasm (the material inside a living cell excluding the nucleus) to synthesize proteins and form replica viruses. Alternatively the RNA can be converted to DNA using a process called reverse transcription. This DNA will be integrated with that of the host DNA in a process similar to a DNA virus.
Coronavirus Genome
- Coronavirus consists of an RNA genome and is one of the largest in the RNA family.
- Coronaviruses are enveloped and contain single-stranded positive-sense RNA. The RNA attaches to the host cell’s ribosome for translation. Positive sense RNA can function as messenger RNA, meaning that viral RNA sequence may be directly translated into the desired viral proteins.
Coronavirus (COVID-19) – Origin and Transmission
- Coronaviruses originate in animals like camels and bats and are zoonotic diseases as it passes from animals to humans occasionally.
- The source of a zoonotic disease is called reservoir species. (For SARS, the reservoir species was identified as bats).
- The first known case of COVID-19 was reported in the Chinese city of Wuhan in December 2019 and was traced to an animal market in the city.
- Research is ongoing on how COVID-19 spreads. However, as per WHO, the disease spreads in humans via exposure to respiratory secretions – the small droplets from the nose or mouth of an infected person – either directly or indirectly.
- The basic reproduction number (R_0) is a measure of transmissibility that aims to describe the average number of people a new case will infect. For COVID-19, WHO estimates R_0 = 1.4 to 2.5. However, many researchers think this figure is under-estimated.
- Compared to earlier outbreaks of SARS and MERS, COVID-19 has a greater global spread and researchers think that mutation in the virus strain is enabling it to be more efficiently transmitted.
Coronavirus (COVID-19) – Clinical Manifestations
- In humans, it affects the upper respiratory tract with varying severity.
- Respiratory infections range from the common cold to bronchiolitis. Pneumonia, gastroenteritis and neurological disorders can also occur.
- Other symptoms are headache, chills, sore throat, and cough.
- The incubation period is from 2 to 5 days and symptoms have a range of 3 to 18 days.
Coronavirus (COVID-19) – Prevention and Treatment

- No vaccine is currently available to prevent COVID-19.
- Avoiding exposure is the only way to prevention. Preventive actions include:
- Avoiding close contact with infected people.
- Avoiding touching eyes, nose, and mouth.
- Staying home when infected and using a facemask.
- Covering while coughing or sneezing.
- Disinfecting frequently touched objects and surfaces.
- No specific antiviral treatment is recommended for COVID-19. Infected people should receive supportive care based on symptoms and for severe cases, treatment should support vital organ functions.
Other Human Coronaviruses
Two other human coronaviruses, MERS-CoV and SARS-CoV were previously identified.
- Middle East Respiratory Syndrome (MERS): MERS cases were reported mainly in the Arabian Peninsula. Symptoms usually include fever, cough, and shortness of breath which often progress to pneumonia. About 3 or 4 out of every 10 patients reported with MERS have died.
- Severe acute respiratory syndrome (SARS): It is believed that the 2003 SARS epidemic started when the virus spread from small mammals in China. SARS symptoms often included fever, chills and body aches which usually progressed to severe pneumonia and breathing difficulty. SARS is more deadly but much less infectious than COVID-19. There have been no outbreaks of SARS anywhere in the world since 2003.
Global Impact of Novel Coronavirus COVID-19
A ‘Pandemic’ is an epidemic that has spread worldwide and is no longer confined to a particular region. COVID-19 is fast approaching pandemic status with many countries implementing pandemic measures.
Economic Impact
- The Coronavirus 2019 has badly impacted the global supply chain.
- COVID-19 emergence coincides with a slowing Chinese economy, growing trade, and tariff-related tensions.
- China is the biggest exporter of intermediate manufactured goods and economies dependent on Chinese imports will be disrupted. For example, Wuhan hosts hundreds of automotive, hardware, electrical equipment, consumer products, and other industries that serve many major manufacturers whose links to the global supply chain now stand severed.
- These are crucial lessons on the importance of having a diversified supply chain.
- China accounts for about 17% of the global GDP and it’s the largest trading partner for most of its neighbors. Economies dependent on China will be hit the hardest.
- Impact on supply chain notwithstanding, other sectors like airlines and tourism are directly impacted. Markets across the world reacted adversely and fears of a global recession have been stoked.
- The SARS pandemic of 2003 is estimated to have caused a global economic loss of $40 billion. COVID-19 will have a more significant impact as the Chinese share of global GDP has quadrupled since then. Some economists estimated that the expected annual losses from pandemic risk to be about $500 billion per year, accounting for both lost income and the intrinsic cost of elevated mortality. (5)
Political Impact
- The COVID-19 episode has resulted in public outrage against the initial cover-up attempts of the Chinese authorities.
- After the initial phase, authoritarian attempts to halt the disease, use of high-tech surveillance, mass quarantine camps and state of lockdown have once again brought forth questions regarding the balance between the freedom of citizens and dealing with a serious national problem.
- The impact on the legitimacy of Chinese President Xi Jinping and the reputation of the Communist Party of China will be judged on how well the crisis will be handled. However, this episode has exposed a systemic weakness in the Chinese top-down model.
Social Impact
- The direct health impact on infected people can be disastrous. Pandemics tend to have a disproportionately higher effect on younger people.
- Shortage of protective equipment and other necessities due to panic buying and hoarding.
- Increase in the burden of health care infrastructure and lack of access to routine health care.
- Sudden population movement due to large-scale disease outbreaks can have destabilizing effects. Migration also compounds the risk of spreading disease.
- The outbreak of infectious diseases can further stigmatize already vulnerable social groups and increase existing social inequalities.
- The spread of rumours and misinformation aided and accelerated by social media makes it harder for people to find reliable guidance.
- Adverse social impact on the people in a state of lockdown.
Public Policy for Handling Pandemics
Following the H1N1 pandemic Influenza, the Government of India issued ‘Clinical management Protocol and Infection Control Guidelines. (7) But an overarching strategy is needed for handling a pandemic in the Indian context where the responsibilities lie divided between the central, state, and local governments.
Case Study 1: Pandemic Interval Framework
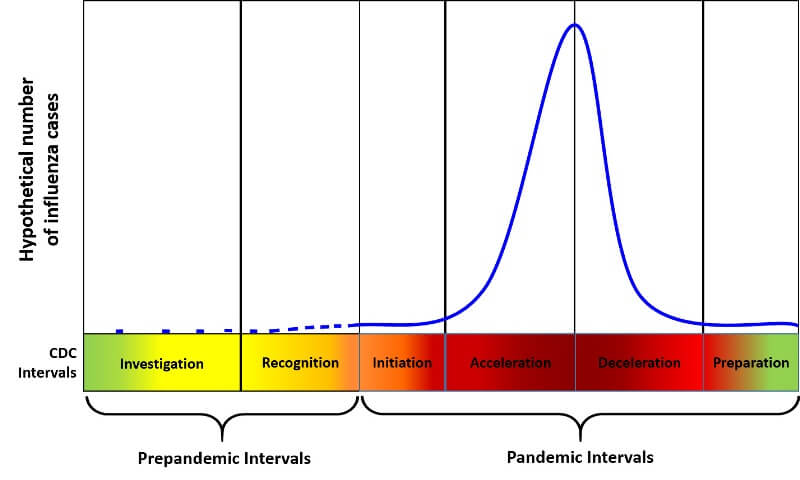
U.S. Centers for Disease Control and Prevention (CDC) has developed a Pandemic Interval Framework (PIF) (8) to guide executives on the kind of public health action required at various stages of the progression of a pandemic. The six intervals and the action to be taken at each interval is summarized below.
Table: Public Health Action at Different Intervals
Intervals |
Public Health Actions |
Investigation of cases of novel virus infection |
|
Recognition of the potential for transmission |
|
Initiation of a pandemic wave |
|
The acceleration of a pandemic wave |
|
Deceleration of a pandemic wave |
|
Preparation for future pandemic waves |
|
Case Study 2: How Kerala Handled Nipah Virus Outbreak
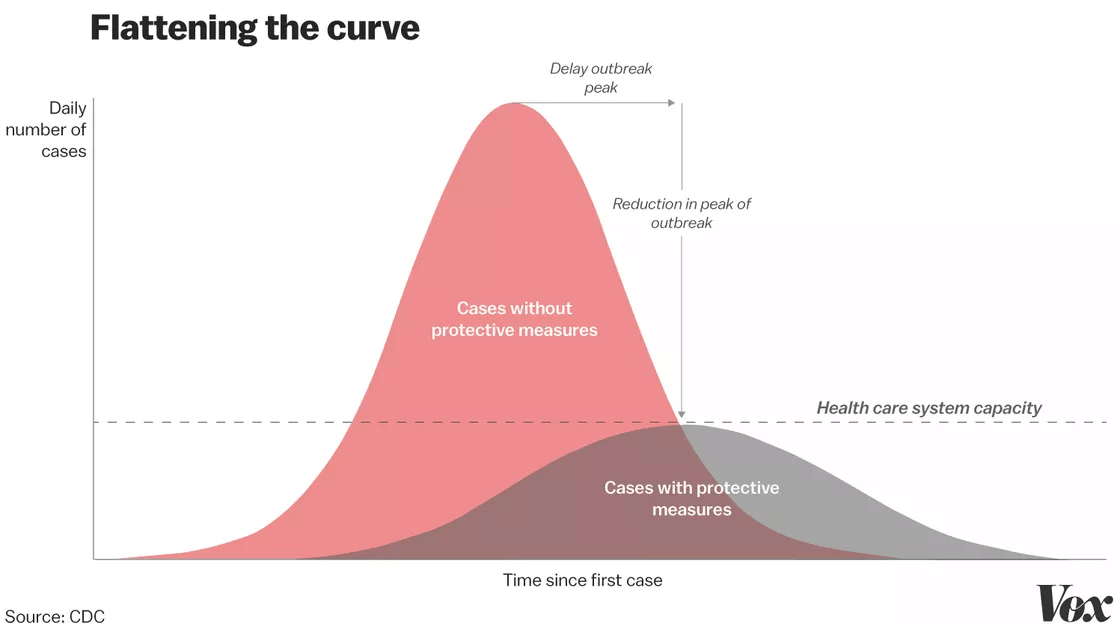
- The Nipah outbreak in Kerala was a serious challenge because of high mortality rates (it killed nearly 70% of those affected during a previous outbreak in Bangladesh), lack of vaccines or specific treatment, and Kerala’s relative inexperience in handling virus outbreaks.
- That the very second case was diagnosed correctly points towards an alert medical community in the state.
- All contacts were traced, surveillance was carried out by a team of medical officials and district administration and potential cases were isolated.
- In this way, every single case reported thereafter was traced back to the first case or its related contacts.
- All contacts of all the cases (around 2000 people) were followed up on a daily basis.
- All suspected cases were moved to the isolation facility set up at Government Medical College, Kozhikode.
- An isolation protocol was established. Health personnel was trained and required safety gear was provided.
- For those infected, anti-viral drugs and life support, measures were provided.
- The state health minister actively supervised these efforts and the outbreak subsided in around five weeks. The deaths were limited to 16.
Case Study 3: China’s use of technology to manage the spread of COVID-19
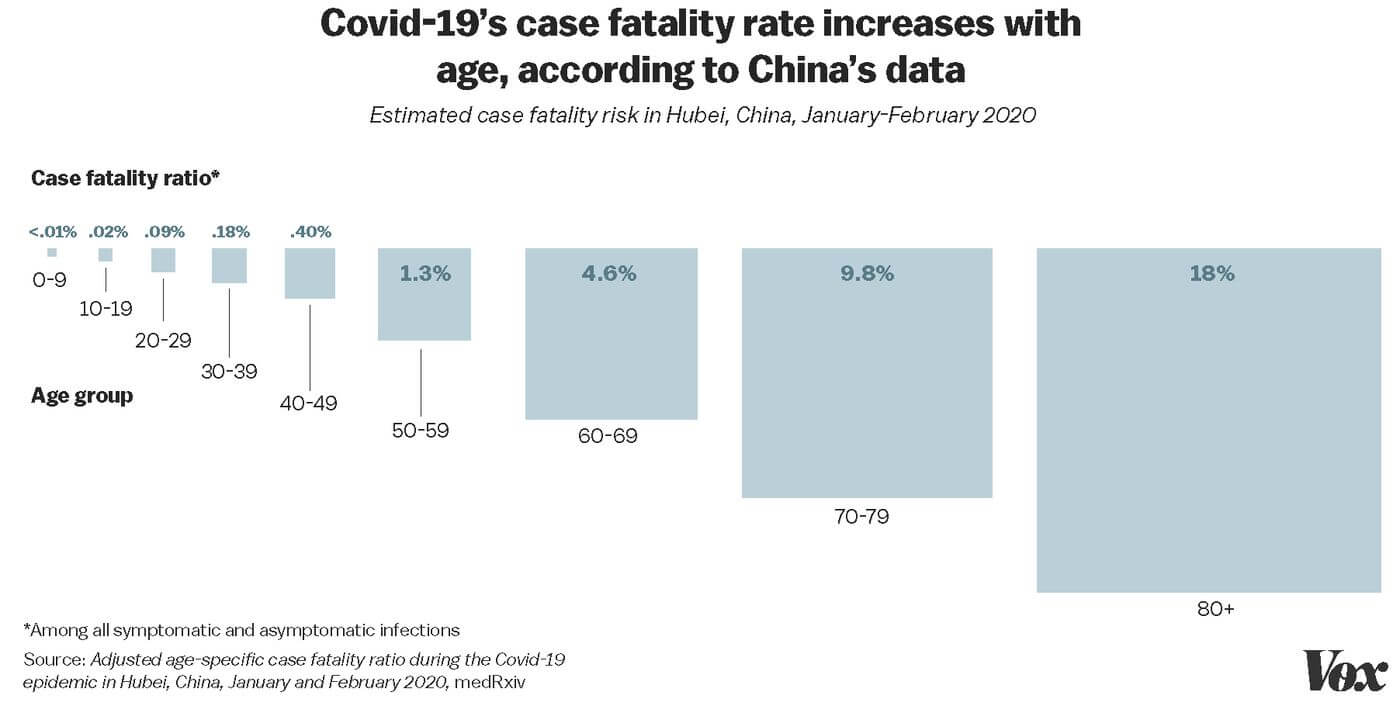
- Aggressive use of surveillance technology by the Chinese government aided by technology companies.
- Tech giants such as Alibaba and Baidu offer Artificial Intelligence (AI) gene sequencing tools.
- Infrared and facial recognition technology to identify and screen travelers.
- AI-enabled temperature measurement using thermal cameras.
- Use of robots and drones to remotely disinfect hospitals, deliver food and enforce quarantine measures.
- Apps that alert users when they are close to infected areas.
- Based on ID numbers and travel history, users of various tech platforms are assigned a QR code that instructs them whether they need to be in quarantine or are free to travel.
Know the difference: Outbreak, Epidemic, and Pandemic
An outbreak is the occurrence of disease cases in excess of what’s normally expected. An epidemic is when there is a sudden increase in reports of a particular disease in a particular area (say a state or country). When an epidemic spreads over several countries or continents it is called a pandemic.
When Coronavirus was limited to Wuhan, it was an outbreak. It became an epidemic when it spread across China. It is now a pandemic as it spreads worldwide.
The Novel Coronavirus Pandemic: Latest statistics
The details about the latest number of confirmed cases on a global level are available from the below links.
Conclusion
India faces a clear and present danger from the spreading of COVID-19.
The central, state, and local governments need to synchronize their actions to identify and isolate potential cases as in the case of the Nipah virus outbreak in Kerala.
Key institutions must be identified as resource centers and to act as nodal points for contact tracing, testing, communications, and case management. Special focus must be on point of entry screening. The use of technology like the Chinese example, but without authoritarian measures, will greatly help in the fight against the virus.
Further, in the long-term perspective, a well-researched pandemic/epidemic management strategy delineating the roles of different authorities and action points at various stages needs to be formulated.
Read: Human metapneumovirus (HMPV): Is it a cause for panic?
Article by Ganesh Kumar V B. The author is a Civil Servant currently working at Madurai. In his free time, Ganesh loves to write about contemporary events of national and international importance.





The article recommends Disinfecting frequently touched objects and surfaces but does not tell how. Please explain how to disinfect touched objects.